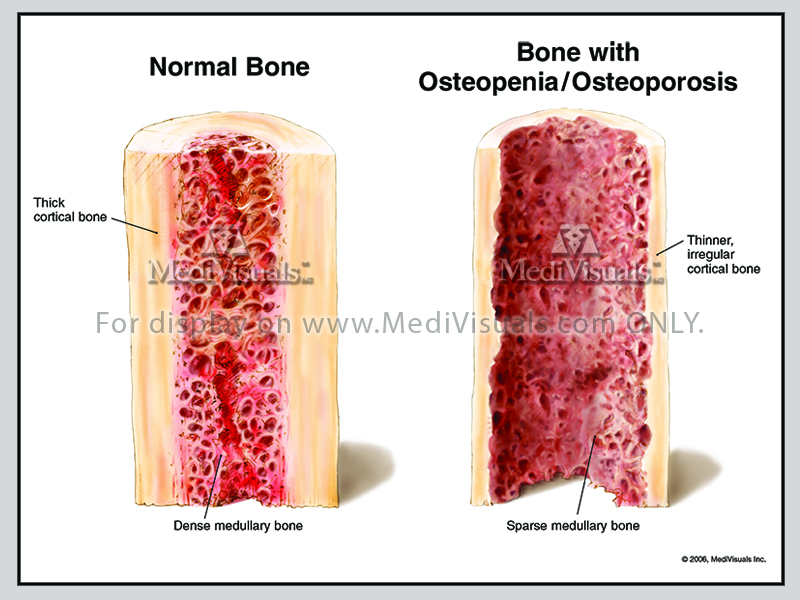
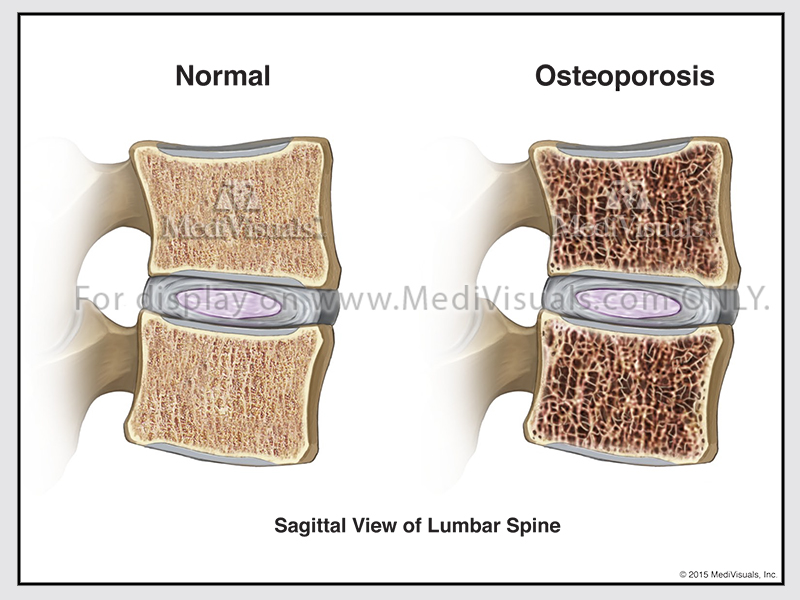
Bone remodeling happens continuously in our bodies. It involves removal of mature bone tissue (bone resorption) and creation of new bone tissue (ossification). These processes also control the healing of fractures. When bone resorption and bone formation are not in balance diseases such as osteoporosis can occur.
New bone is created by osteoblast cells, while osteoclast cells break down bone. Remodeling of bones requires calcium and a balance between the function of these two types of cells. Chemical signals in the body cause osteoclasts to move to an area and breakdown bone, followed by osteoblasts creating new bone in the area.
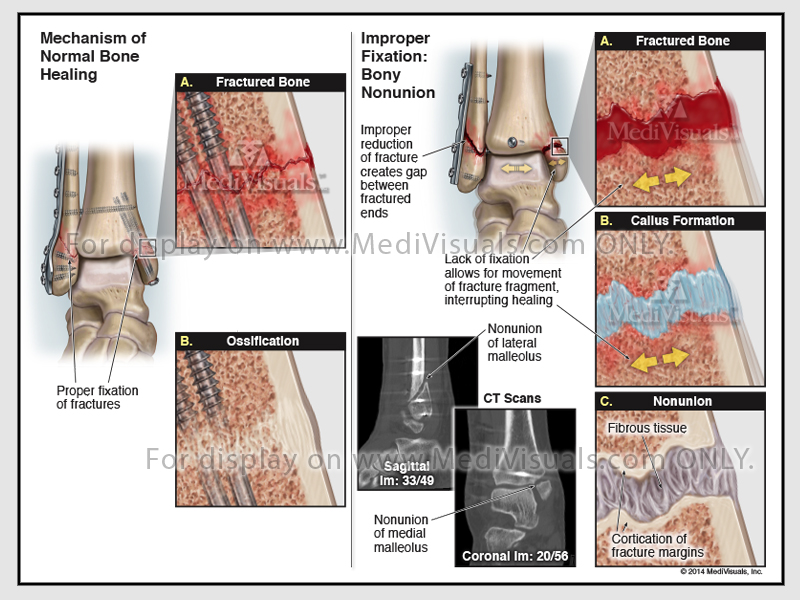
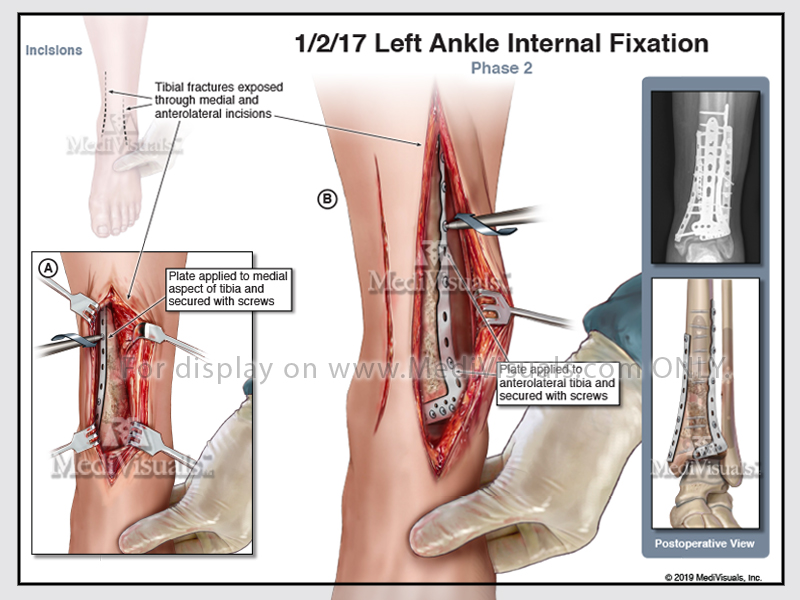
Clinical treatment of bone fractures requires realignment of the dislocated bone fragments and then fixation with a cast or hardware to keep them from moving so the healing process can occur. Healing begins in the vascularized periosteum (the connective tissue membrane covering the bone) and in bone marrow. The periosteum and bone marrow are areas where precursor cells become chondroblasts and osteoblasts, essential to the healing of bone.
The three major phases of fracture healing are the Inflammatory Phase, the Reparative Phase, and the Remodeling Phase.
Inflammatory Phase
After a fracture, blood accumulates within the tissues adjacent to the injury (hematoma). Cells within this blood clot die, but fibroblast cells survive and replicate. They form granulation tissue (a grouping of these new cells, with blood vessels in between).
Reparative Phase
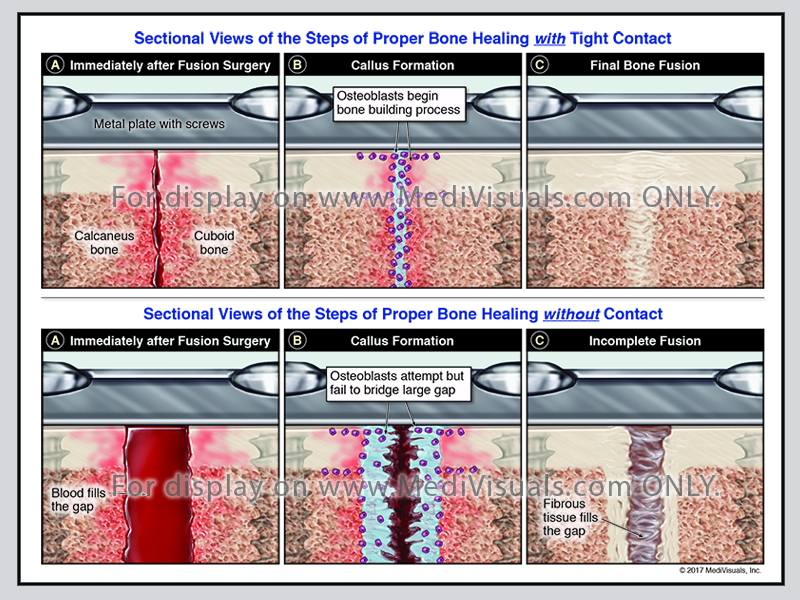
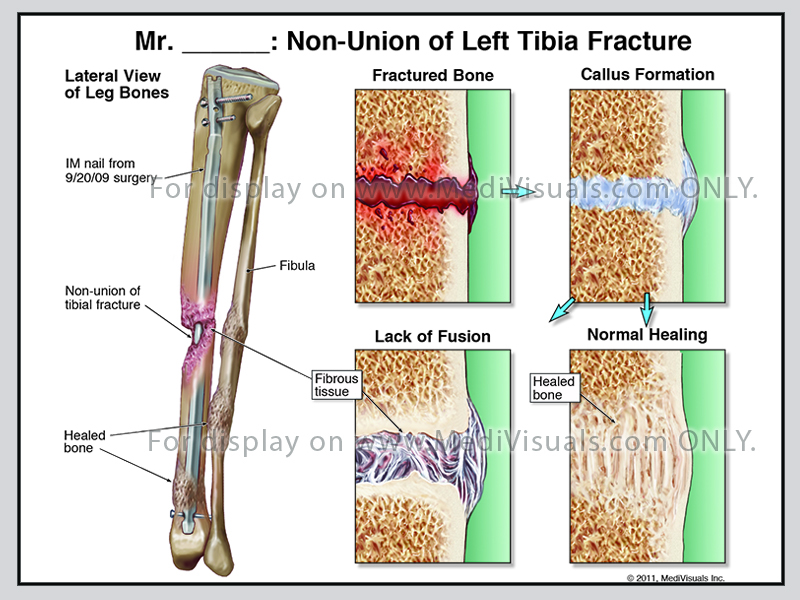
Days after the fracture, the cells of the periosteum replicate and form chondroblasts that create cartilage, and osteoblasts that create woven bone. These tissues come together and form a callus. This initial “woven” bone is not as strong as mature bone.
Remodeling Phase
The remodeling process replaces the woven (trabecular) bone with stronger mature
(cortical) bone. The callus is remodeled into a new shape closer to the bone’s original shape and strength due to mechanical loading forces. The remodeling phase takes 3 to 5 years. Fibroblasts lay down a collagen matrix. Calcium is added to the collagen matrix and stiffens it into mature bone.
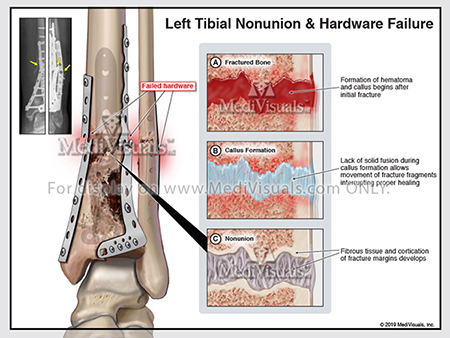
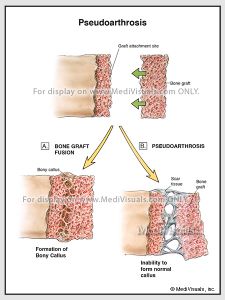
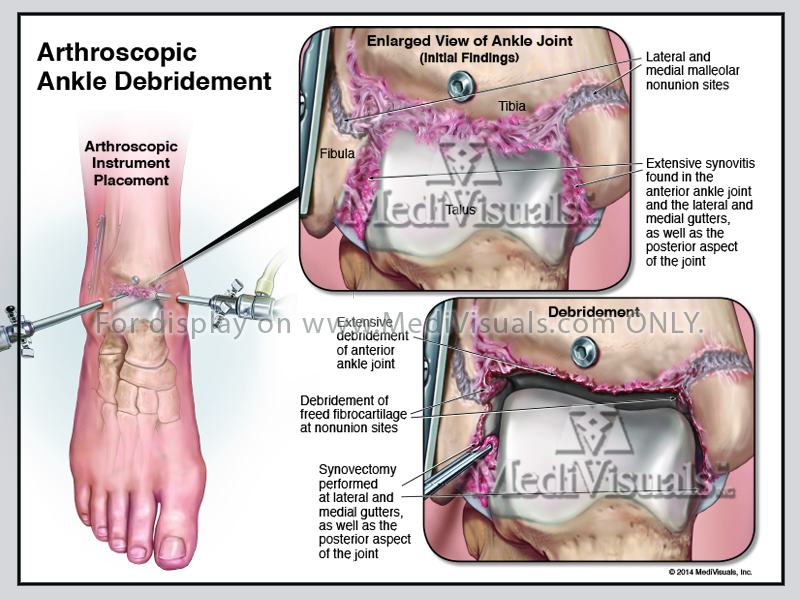
Improper fracture healing includes delayed union, non-union, and fibrous union. If the periosteum and the blood supply are disrupted, fracture healing can be delayed and may not fully heal (non-union). Inappropriate fixation of the bone fragments can also result in improper healing. Non-union can result in gaps between healing fragments, and the formation of unstable fibrous tissue between fragments. Gaps between the bone fragments can sometimes appear to be a “false joint” and are called pseudoarthosis. Non-union may require additional surgical intervention to remove the fibrous tissues, restore the blood supply, and perhaps add bone graft between fragments to ensure proper healing.